STUDY SHEDS LIGHT ON THE TREATMENT OF ASYMPTOMATIC CAROTID STENOSIS
January 2026
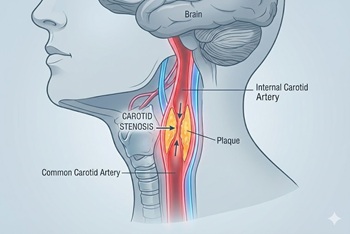
For decades, clinicians have debated the optimal management of asymptomatic high-grade carotid stenosis. While revascularization (stenting or endarterectomy) is often performed to prevent future strokes, previous trials comparing these interventions to medical therapy are outdated, predating the era of high-intensity statins and aggressive blood pressure control. To determine if revascularization provides a benefit over modern pharmacotherapy, researchers conducted CREST-2, a pair of parallel, multicenter, randomized trials involving 2,485 patients with severe asymptomatic carotid stenosis (≥70%).
In the study, all participants received intensive medical management (IMM) involving lifestyle coaching and pharmacotherapy targeting a systolic blood pressure <130 mm Hg and an LDL cholesterol <70 mg/dL. Patients were then randomized into two distinct trials based on their suitability for revascularization type: one comparing carotid artery stenting (CAS) plus IMM versus IMM alone (n=1,245), and another comparing carotid endarterectomy (CEA) plus IMM versus IMM alone (n=1,240). The primary outcome was a composite of perioperative stroke or death (within 44 days) or ipsilateral ischemic stroke up to 4 years. The results were as follows:
- CAS Trial Primary Outcome: CAS group - 2.8% vs. IMM group - 6.0% (P=0.02)
- CEA Trial Primary Outcome: CEA group - 3.7% vs. IMM group - 5.3% (P=0.24)
- Periprocedural Safety (Stroke/Death): CAS - 1.3%, CEA - 1.5%, Medical Management - 0%
The CREST-2 study suggests that the benefit of revascularization for asymptomatic carotid stenosis depends heavily on the modality used. Carotid stenting combined with intensive medical management significantly reduced the risk of stroke or death compared to medical management alone. Conversely, carotid endarterectomy did not demonstrate a statistically significant benefit over medical therapy.
Perhaps the most clinically relevant finding from CREST-2 is the low rate of stroke in the medically managed groups (approximately 1.3% to 1.7% annualized rate). These rates are markedly lower than those seen in historical trials, confirming that modern, aggressive management of blood pressure and lipids is highly effective at stabilizing plaque and preventing events. This poses a challenge to the "fix it" reflex; while stenting offered a relative risk reduction, the absolute risk difference was modest. Furthermore, any procedural intervention carries an upfront risk of periprocedural stroke or death (1.3% to 1.5% in this study).
These findings support a nuanced approach to patient care. For patients with asymptomatic disease who are good candidates for stenting and have a reasonable life expectancy, CAS offers a durable advantage. However, for patients who are surgical candidates or those preferring a conservative approach, intensive medical management alone is a safe and robust strategy, provided that strict targets for blood pressure and lipids are achieved.
