
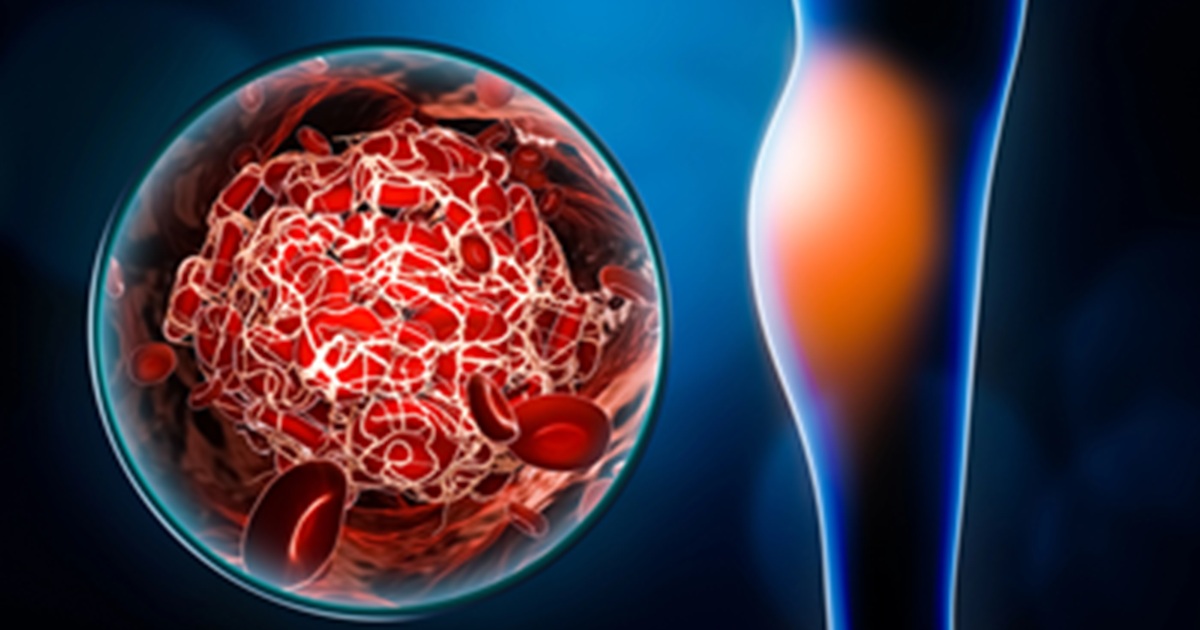
Trial found modest symptom improvement but increased bleeding risk with venous stenting
The issue: Post-thrombotic syndrome (PTS) can cause chronic limb symptoms after DVT. Effective PTS therapies are lacking.
Why this study matters: Evaluated the effects of iliac vein stent placement for PTS
Primary care relevance: Offers guidance on counseling patients with PTS who are considering endovascular therapy
April 2026
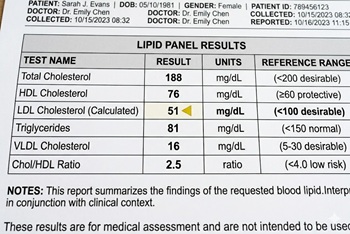
The Ez-PAVE trial randomized patients with cardiovascular disease (CVD) to an LDL target of less than 55 mg/dL versus less than 70 mg/dL
The issue: Recent American Heart Association (AHA) cholesterol treatment guidelines include an optional, stricter LDL target of less than 55 mg/dl for patients at very high risk for recurrent cardiovascular events. Studies evaluating target levels this low are lacking.
Why this study matters: The Ez-PAVE trial evaluated the effects of an LDL target below 55 mg/dL versus below 70 mg/dL in patients with CVD
Primary care relevance: The trial provides clinical evidence on the effects of targeting very low LDL cholesterol levels
April 2026
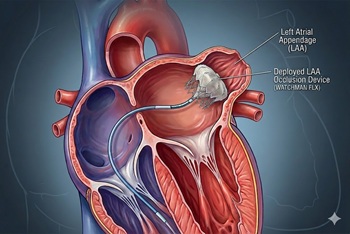
Unlike previous trials, LAAC did not perform as well in the CLOSURE-AF trial, which enrolled high-risk patients
The issue: Left atrial appendage closure (LAAC) has been viewed as an alternative to long-term anticoagulation in atrial fibrillation, particularly when bleeding risk is high.
Why this study matters: The CLOSURE-AF trial randomized patients at high risk for stroke and bleeding to LAAC or physician-directed therapy (mostly DOACs); LAAC was not noninferior for the primary composite endpoint over a median of 3 years.
Primary care relevance: Reinforces that LAAC is not a one-size-fits-all substitute for anticoagulation in the highest-risk multimorbid patients; perioperative antithrombotic needs and complications matter in shared decision-making.
March 2026
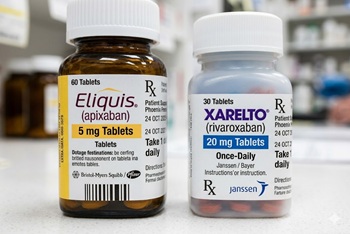
COBBRA trial shows lower bleeding risk with apixaban over 3 months without increased recurrent VTE
The issue: Apixaban and rivaroxaban are both widely used for acute VTE, but large randomized trials comparing their effects are lacking
Why this study matters: The COBBRA trial compared apixaban to rivaroxaban for the treatment of acute symptomatic venous thromboembolism
Primary care relevance: Study provides comparative evidence on apixaban and rivaroxaban for acute VTE
March 2026

The 2026 update is the first significant update in eight years, replacing the 2018 guidelines
The issue: Eight years after the prior update, major lipid-management recommendations have changed, including earlier screening and more aggressive LDL-C targets.
Why this matters: The 2026 guideline emphasizes PREVENT-based risk assessment, routine one-time Lp(a) testing, and faster use of combination lipid-lowering therapy in high-risk patients.
Primary care relevance: Primary care clinicians should shift to PREVENT equations, expand risk-stratification with Lp(a)/ApoB, and escalate beyond statins when LDL-C and non-HDL-C goals are not reached.
March 2026
Intranasal etripamil (Cardamyst) offers a new self-administered option for rapid PSVT conversion in select patients
The issue: Vagal maneuvers are first-line for stable acute SVT, but real-world conversion rates range from 5 to 20%, and many patients still seek emergency care.
Why this matters: In its pivotal trial, Cardamyst (etripamil) converted AV-nodal-dependent PSVT within 30 minutes in 64% of patients vs 31% with placebo
Primary care relevance: Cardamyst provides an at-home, symptom-prompted option for selected adults who want episodic control of SVT, possibly decreasing emergency department visits and deferring catheter ablation.
March 2026
STABLED trial found no benefit of adding catheter ablation to edoxaban in patients with AF and recent stroke
The issue: Catheter ablation is widely used for atrial fibrillation; whether adding it to anticoagulation improves hard outcomes in high-risk patients, such as those with a recent stroke, is uncertain.
Why this study matters: It evaluated the safety and efficacy of adding catheter ablation to anticoagulation in patients with AF and recent stroke.
Primary care relevance: Provides information for counseling patients about the benefits and risks of catheter ablation.
February 2026

Individual-patient-data meta-analysis finds no benefit of beta-blockers after MI in patients with preserved ejection fraction
The issue: Four large trials evaluating the benefits of beta-blockers in post-MI patients with preserved LVEF came to different conclusions
Why this study matters: It combines data from the trials and offers an estimate of the overall effect of beta-blockers in this patient population.
Primary care relevance: Supports reassessing the need for long-term beta-blockers in post-MI patients with preserved EF.
February 2026
PISCES trial finds fish oil reduces cardiovascular events in hemodialysis patients
The issue: Large trials of fish oil for CVD prevention have yielded conflicting results; REDUCE-IT showed benefit while STRENGTH did not.
Why this study matters: The PISCES trial randomized 1,228 hemodialysis patients to fish oil 4 g daily or corn-oil placebo; fish oil reduced serious cardiovascular events by 43% (HR 0.57; 95% CI, 0.47 to 0.70; P<0.001) over 3.5 years.
Primary care relevance: PISCES aligns with REDUCE-IT but contradicts STRENGTH; the overall effects of fish oil on CVD remain inconclusive.
January 2026

Two randomized trials examine whether anticoagulation can be safely discontinued after successful catheter ablation
The issue: One-year success rates of catheter ablation for atrial fibrillation range from 50 - 85% and decline over time. Many patients hope to stop anticoagulation after ablation, but the risks and benefits of this decision have not been clearly defined.
Why these studies matter: The ALONE-AF and OCEAN studies were designed to evaluate the risks and benefits of stopping anticoagulation after successful catheter ablation. They also provided guidance on what defines successful ablation.
Primary care relevance: The studies provide data for making an informed decision on stopping anticoagulation and determining which patients are candidates.
January 2026
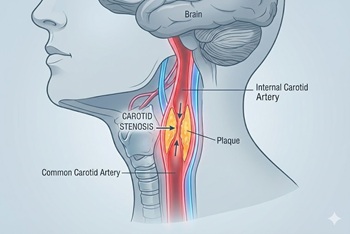
New randomized trial compares carotid stenting and endarterectomy to intensive medical management
The issue: In the U.S., most asymptomatic high-grade (≥70%) carotid stenosis is treated with revascularization (stenting or endarterectomy). However, the risks and benefits of this approach, and how it compares with contemporary medical therapy, have never been evaluated in a clinical trial.
Why this study matters: The CREST-2 study provides the first modern evidence comparing carotid stenting and endarterectomy to intensive medical management for asymptomatic carotid stenosis.
Primary care relevance: Providers now have good data to counsel patients on the risks and benefits of stenting, endarterectomy, and medical management of asymptomatic carotid stenosis.
December 2025

DECAF trial challenges long-standing recommendations to avoid coffee
The issue: Patients with atrial fibrillation are routinely advised to avoid caffeinated beverages, but evidence supporting this recommendation has been inconsistent.
Why this study matters: The DECAF randomized clinical trial compared continuing caffeinated coffee consumption to abstinence in patients with atrial fibrillation who underwent successful electrical cardioversion.
Primary care relevance: Provides guidance on counseling patients with atrial fibrillation about coffee consumption.
November 2025
Recent trials question routine long-term beta-blocker use after MI
The issue: Beta-blockers are routinely recommended for all post-MI patients, but this practice is based on trials predating modern revascularization and intensive secondary prevention.
Why this study matters: Four recent randomized trials have evaluated the long-term benefit of beta-blockers in post-MI patients with preserved LVEF.
Primary care relevance: Provides guidance on continuing beta-blockers in post-MI patients with preserved LVEF.
October 2025
The HI-PRO trial randomized patients with provoked VTE and minor chronic risk factors to 12 months of apixaban or placebo after completing at least 3 months of anticoagulation.
The issue: Current guidelines recommend 3 months of anticoagulation for provoked VTE; the role of extended therapy in patients with ongoing risk factors is unclear.
Why this study matters: The trial evaluated the long-term benefit of extended anticoagulation in patients with provoked VTE and minor chronic risk factors.
Primary care relevance: Provides guidance on extending anticoagulation in patients with provoked VTE and minor chronic risk factors.
October 2025
Study finds higher potassium targets are beneficial in patients with ICDs and CVD
The issue: Patients with ICDs and cardiovascular disease are at risk for ventricular arrhythmias; potassium levels may influence this risk.
Why this study matters: The trial evaluated the benefit of targeting high-normal potassium levels (4.5–5.0 mEq/L) in patients with ICDs and CVD.
Primary care relevance: Provides guidance on adjusting potassium supplements and medications in patients with ICDs and CVD.
September 2025
The guidelines are thorough, but are they practical?
The issue: Primary aldosteronism is an underdiagnosed cause of hypertension; screening and confirmatory testing vary in practice.
Primary care relevance: Updated guidance helps identify patients with resistant or hypokalemic hypertension who may benefit from screening and targeted treatment.
July 2025
First non-SGLT2 inhibitor approved for HFpEF
The issue: HFpEF has limited pharmacologic options; SGLT2 inhibitors are approved but additional therapies are needed.
Why this study matters: Finerenone (Kerendia), a nonsteroidal mineralocorticoid receptor antagonist, was approved for HFpEF based on the FINEARTS-HF study, showing reduced worsening heart failure events.
Primary care relevance: Providers now have a third drug option for HFpEF and the first non-SGLT2 inhibitor for this condition.
June 2025
Albumin-adjusted calcium formulas are less accurate than unadjusted levels for calcium status
The issue: Corrected (albumin-adjusted) calcium is widely used in hypoalbuminemia, but accuracy has been questioned.
Why this study matters: It evaluates the accuracy of albumin-adjusted calcium formulas for determining calcium status.
Primary care relevance: Relying on corrected calcium may be misleading; unadjusted levels or ionized calcium may be more reliable when assessing calcium status.
May 2025
Another study finds clopidogrel is better than aspirin in South Koreans with chronic coronary disease
The issue: Antiplatelet choice for chronic coronary disease remains debated; aspirin has been standard but clopidogrel has been compared in several trials.
Why this study matters: A trial in South Korean patients with CCD found clopidogrel superior to aspirin for cardiovascular outcomes.
Primary care relevance: Adds to the evidence base for antiplatelet selection in chronic coronary disease; although applicability may vary by population.
April 2025

The SOUL Study is a larger and longer version of a previous Rybelsus trial
The issue: Wegovy has been shown to reduce cardiovascular events in type 2 diabetes; the effects of Rybelsus are unknown.
Why this study matters: The SOUL study evaluated the long-term benefit of Rybelsus in adults with type 2 diabetes and established or high cardiovascular risk.
Primary care relevance: Provides evidence on the benefits of Rybelsus for preventing cardiovascular events in patients with type 2 diabetes and established or high cardiovascular risk.
December 2024
BPROAD found intensive BP control reduced CVD in type 2 diabetes, contradicting ACCORD
The issue: Optimal blood pressure targets in type 2 diabetes have been debated; ACCORD suggested no benefit from intensive control, but newer evidence was needed.
Why this study matters: The BPROAD study found that intensive BP control (systolic <120 mmHg) significantly reduced cardiovascular disease in type 2 diabetes, contradicting the older ACCORD trial.
Primary care relevance: Updated evidence supports consideration of intensive BP targets in some patients with type 2 diabetes; guidelines may evolve.
December 2024

CLEAR study: colchicine failed to improve CVD outcomes in recent MI patients after PCI
The issue: Prior trials suggested colchicine could reduce cardiovascular events; the CLEAR study tested this in a different population.
Why this study matters: Despite prior positive studies, colchicine did not improve CVD outcomes in the CLEAR study, which included patients with recent MI who had undergone PCI; high dropout and factorial design may explain discrepant findings.
Primary care relevance: Colchicine for secondary CVD prevention is not supported by this trial; existing guidance may need to be revisited.
December 2024
Cross-sectional study finds secondary hypertension prevalent in 30% of hypertensive adults aged 18–40
The issue: Secondary hypertension is often underdiagnosed; prevalence in young adults was unclear.
Why this study matters: A cross-sectional study found secondary hypertension in about 30% of hypertensive adults aged 18 to 40, highlighting the importance of screening in younger patients.
Primary care relevance: Young adults with hypertension may warrant a higher index of suspicion for secondary causes and appropriate workup.